What Causes Spider Veins: Risks, Prevention, and Treatments
- Mar 19
- 11 min read
Have you ever noticed fine, web-like lines appearing on your legs and wondered where they came from? You're not alone. Spider veins are tiny, damaged veins near the skin's surface that become visible when blood pools inside them. This happens because the miniature one-way valves within the veins get weak, disrupting blood flow and creating those familiar patterns. Think of it like a small traffic jam happening just beneath your skin.
At Mid-County Dermatology, our board-certified dermatologists, Dr. Feigenbaum and Dr. Gibstine, help patients across St. Louis understand what causes spider veins and how to manage them effectively.
What You Need to Know: A Quick Overview
What are they? Spider veins are small, damaged veins visible on the skin's surface, usually red, blue, or purple.
What's the main cause? The direct cause is weakened or damaged valves inside the veins, a condition known as venous insufficiency.
What are the biggest risk factors? Genetics, hormonal changes (like pregnancy and menopause), aging, prolonged standing or sitting, and excess weight.
Are they dangerous? For most people, spider veins are a cosmetic issue. However, if accompanied by pain, swelling, or skin changes, they can indicate a deeper medical condition.
Can they be treated? Yes, effective treatments like sclerotherapy and laser therapy are available from a qualified St. Louis dermatologist.
Why Do Spider Veins Appear?
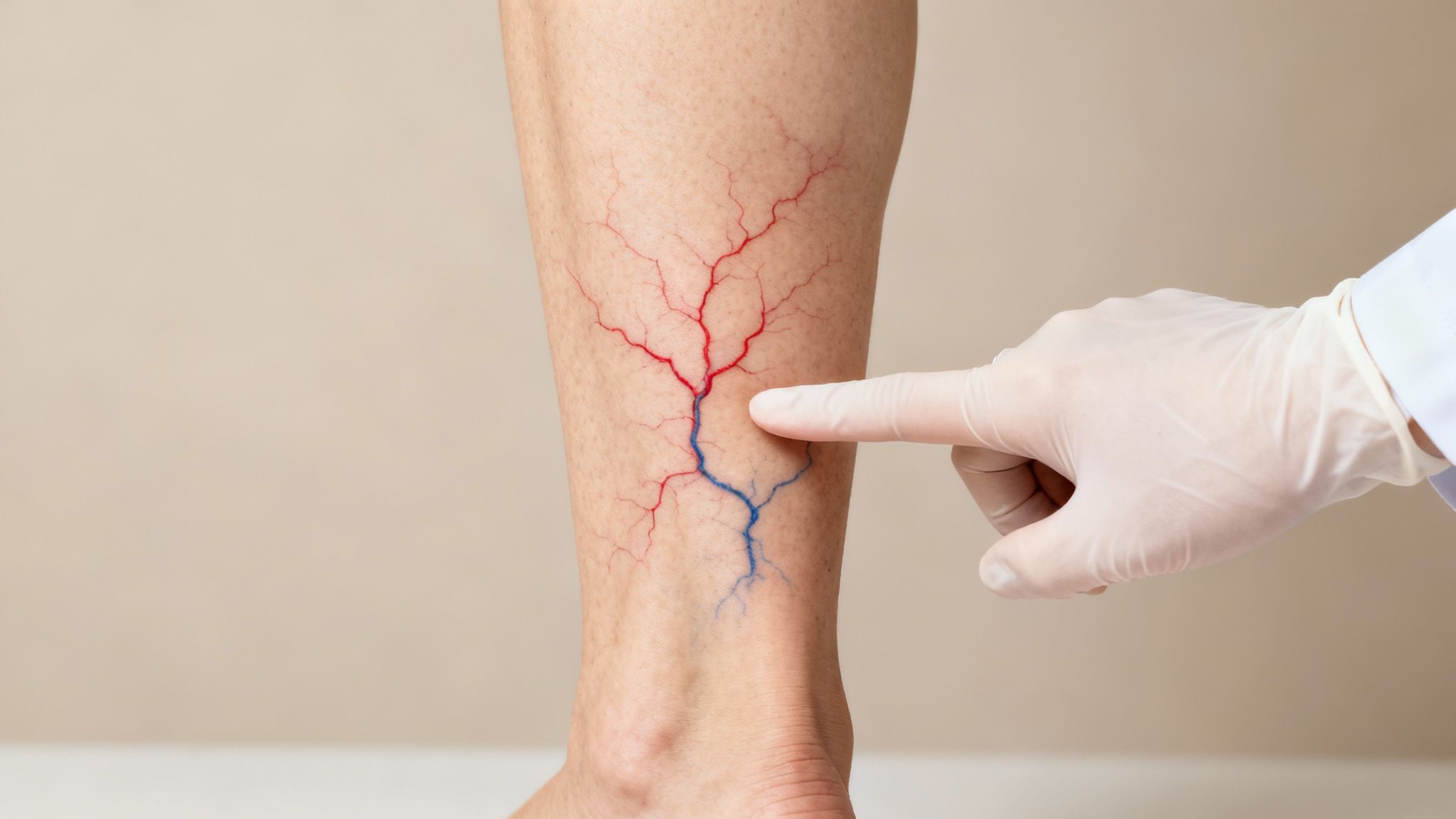
If you've spotted these fine lines, you're in good company. Medically known as telangiectasias, spider veins are incredibly common. A study published in StatPearls (2023) showed that up to 88% of women and 79% of men may have them.
Despite being widespread, for most people they are a cosmetic concern, not a sign of a serious medical problem. You can read the full research about these findings.
Here at Mid-County Dermatology, Dr. Feigenbaum and Dr. Gibstine often explain the key difference between what directly causes a spider vein and the other factors that increase your risk. Getting a handle on this distinction is the first step in managing your vein health, whether you live in Ladue, Clayton, or anywhere else in the St. Louis area.
Primary Causes vs. Contributing Risk Factors for Spider Veins
The appearance of spider veins isn’t random. It’s the result of a specific mechanical failure inside your veins, often accelerated by lifestyle and genetic factors. A St. Louis dermatologist can help you pinpoint which factors might be playing the biggest role for you.
To make this clearer, let's break down the direct causes versus the contributing risk factors.
Factor Type | Description | Examples |
|---|---|---|
Primary Cause | This is the direct, physical reason the veins become visible—the "what" that's happening inside your body. | Venous Insufficiency: This is the technical term for when tiny, one-way valves in your veins weaken. They can't stop blood from flowing backward and pooling, which makes the vein swell and become visible. |
Contributing Risk Factor | These are the conditions or habits that make valve failure more likely to happen. Think of these as the "why" it might be happening to you. | Genetics, hormonal shifts (pregnancy, menopause), prolonged standing/sitting, aging, and excess weight. |
Essentially, the primary cause is the faulty valve itself. The risk factors are all the things that put extra strain on those valves, making them more likely to give out over time.
As a leading St. Louis skin specialist practice, we help patients from Creve Coeur to Chesterfield understand this relationship. This allows us to build prevention and treatment plans that actually work.
How Your Veins Work and Where Things Go Wrong
To really get what causes spider veins, it helps to understand the incredible plumbing system working inside your legs. Your veins are a complex network of one-way streets designed to get blood from your feet back up to your heart, against gravity.
Lining these streets are tiny, flap-like gates called valves. When your leg muscles squeeze, they push blood upward, and the valves open. A moment later, they snap shut, stopping gravity from pulling the blood right back down. It's a beautifully efficient system.
The Breakdown in the System
The trouble starts when these hardworking valves wear out or get damaged. Imagine those one-way gates getting a little rusty and failing to close completely. Now, blood can leak backward and start to pool where it shouldn't.
This backward flow is what doctors call venous insufficiency or venous reflux. As blood collects, the pressure inside that section of the vein starts to build. This single issue is the root cause of most vein problems.
"At its core, a spider vein is a sign of localized pressure overload," explains Dr. Feigenbaum of Mid-County Dermatology. "The larger, deeper veins can often handle this pressure, but the delicate capillaries just beneath the skin can't. They expand and dilate under the strain, which is what makes them visible."
From Pressure to Visible Veins
This built-up pressure has to go somewhere, and it often gets forced into the smaller, more delicate veins just under your skin's surface. These tiny vessels, technically known as telangiectasias, simply aren't designed to handle that kind of load.
As they stretch and swell with backed-up blood, they pop into view as the fine red, blue, or purple webs we know as spider veins. This is why anything that increases pressure in your legs—like standing all day for your job or carrying extra weight—is a major risk factor.
For our patients in Frontenac and Chesterfield, grasping this simple mechanical failure is the first step toward a solution. As a premier St. Louis Dermatology practice, our job is to demystify these common conditions.
The Key Factors That Increase Your Risk
So, we know a tiny, failing valve is the direct mechanical culprit. But that failure doesn't just happen in a vacuum. A number of factors can put extra stress on your circulatory system, making these delicate valves much more likely to weaken.
Getting a handle on these influences is the first step. It helps you separate what you can control from what you can’t, giving you the power to be proactive about prevention.
This graphic gives you a clear visual of how a healthy vein can turn into a spider vein once a valve gives out.
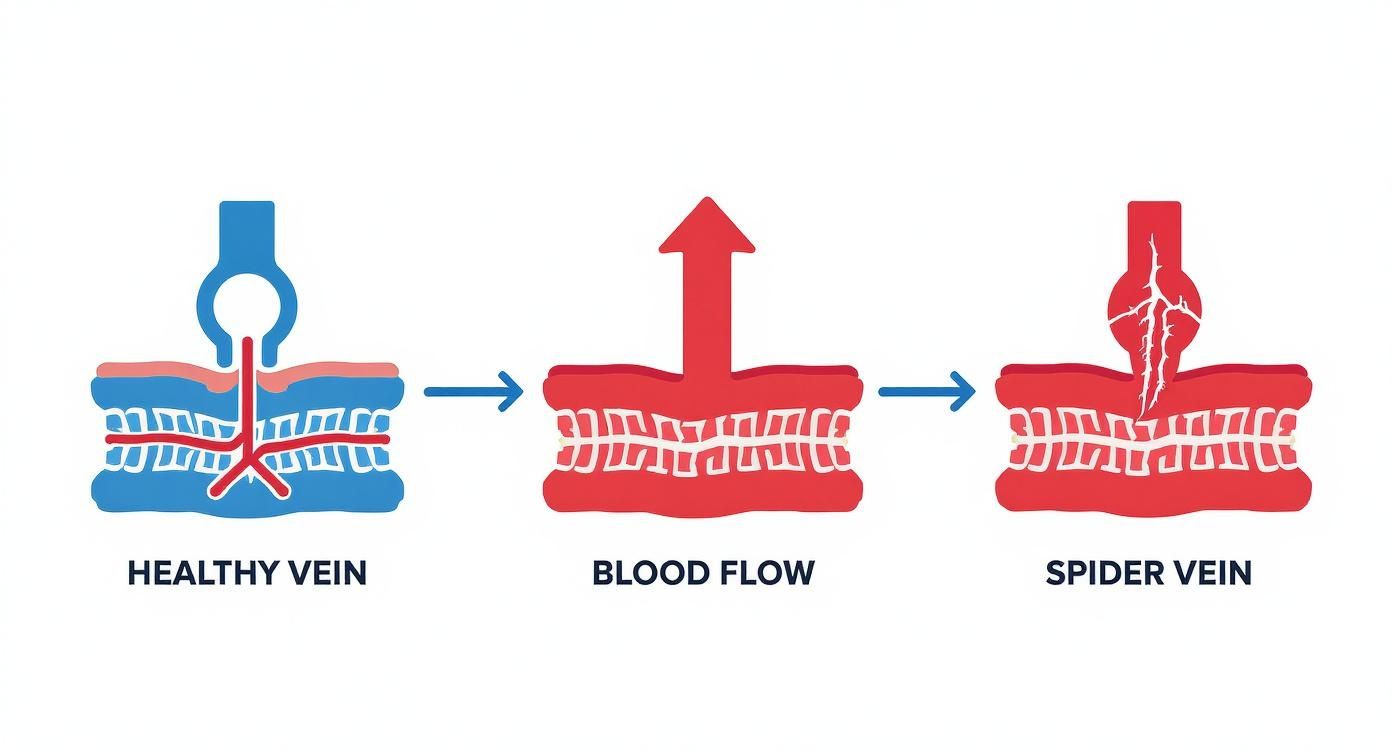
As you can see, the process breaks down when the valve can no longer stop blood from flowing backward. That leads to pooling, pressure, and those tiny veins becoming visible.
Genetic Predisposition
Honestly, one of the most significant factors is your family tree. If your parents or grandparents had spider veins, your odds of developing them are much higher. In fact, research cited by the American Academy of Dermatology (AAD) suggests that up to 90% of people with spider veins have a family history of them.
You might inherit vein walls or valves that are naturally weaker. You can't change your genes, but knowing this risk is in your background can empower you to be more vigilant with preventative lifestyle choices.
Hormonal Fluctuations
Hormones—especially estrogen and progesterone—play a surprisingly big part in vein health. These hormones can relax the walls of your veins, which may affect how well the valves close.
This hormonal link is a key reason women are more prone to spider veins, particularly during certain life stages:
Pregnancy: A surge in blood volume and hormones puts immense pressure on leg veins.
Menopause: Shifting hormone levels can impact vein elasticity and strength.
Birth Control: For some women, hormonal contraceptives can also be a contributing factor.
Since this is a common trigger, looking into ways to support a healthy [hormone balance for women](https://vitzai.com/blogs/learn/hormone-balance-supplements-for-women) can be a smart, proactive step.
Lifestyle and Occupational Habits
Your day-to-day routine can either help or hinder your venous system. Two of the biggest lifestyle culprits are spending long stretches of time either standing or sitting, and carrying excess body weight.
Jobs that keep you on your feet all day—a reality for many nurses, teachers, and service industry workers in the St. Louis area—force your veins to work overtime. On the flip side, sitting at a desk for hours can be just as bad, slowing down circulation.
At our St. Louis dermatology practice, Dr. Gibstine often advises patients from Clayton to Chesterfield on simple workplace adjustments. "Even small changes, like taking brief walking breaks or elevating your feet, can make a meaningful difference in reducing leg vein pressure over a lifetime."
Excess weight also adds tremendous pressure to your lower body, and your veins feel that strain. Over time, this constant pressure can weaken valves. As noted in a 2014 study in Circulation, venous diseases affect a huge portion of the population, with milder forms like spider veins impacting up to 60% of all adults.
Debunking Common Spider Vein Myths
There’s a lot of misinformation out there about spider veins. As a trusted St. Louis skin doctor practice, our team at Mid-County Dermatology is here to help separate fact from fiction.
Knowing what doesn't cause spider veins is just as important as knowing what does.
Spider Vein Myth vs. Fact
We hear these common beliefs from patients all over St. Louis, from Ladue to Creve Coeur. Here's what our board-certified dermatologists, Dr. Feigenbaum and Dr. Gibstine, want you to know.
Common Myth | The Fact (Evidence-Based) |
|---|---|
Crossing your legs causes spider veins. | False. According to the American Academy of Dermatology (AAD), crossing your legs does not cause spider veins. While it can temporarily affect circulation, it doesn't create enough pressure to damage vein valves. The real culprits are genetics, hormones, and prolonged standing or sitting. |
Only older people get spider veins. | Not true. While risk increases with age as veins lose elasticity, spider veins can appear at any age. We often see them in younger patients, especially those with a strong family history or during pregnancy. |
Spider veins are always a sign of a serious health problem. | Usually, they are not. For most people, spider veins are a cosmetic concern and not dangerous. However, if they come with symptoms like aching, swelling, or skin changes, it could point to underlying venous insufficiency that needs a professional evaluation. |
Clarifying Common Misconceptions
It's easy to get confused by online "health tips." For instance, some people assume any visible red lines on the face are spider veins, but they could be related to other conditions. Understanding the differences between conditions like rosacea vs. acne can help pinpoint the real source of facial redness.
A key takeaway is that spider veins are a circulation issue rooted in vein valve function. They are not a skin-deep problem caused by surface-level actions like crossing your legs or getting a tan.
Another common myth is that you can "cure" spider veins with special creams. No topical cream can repair a damaged vein valve. Effective treatment requires a medical procedure, like sclerotherapy or laser therapy, performed by a qualified St. Louis skin specialist.
Practical Steps for Vein Health and Prevention

While you can't change your genes, you can absolutely influence your venous health through proactive lifestyle choices. Taking simple, consistent steps can support your circulation, reduce pressure on your leg veins, and potentially slow the formation of new spider veins.
Think of these actions not as a cure, but as a powerful long-term strategy for managing your risks. Studies have shown the prevalence of venous disorders varies dramatically. Up to 85% of women and 80% of men in Western countries develop some form of venous issue, while being much rarer in other parts of the world, highlighting the impact of lifestyle. You can discover more insights about these geographic differences on AHA Journals.
Actionable Steps for Stronger Veins
Here are some manageable adjustments recommended by our St. Louis dermatologists:
Get Moving Regularly: Low-impact exercises like walking, swimming, or cycling are fantastic for your veins. These activities engage your calf muscles, which act as a powerful pump to help push blood back up toward your heart.
Maintain a Healthy Weight: Excess weight puts constant, direct pressure on the veins in your legs. Managing your weight is one of the most effective ways to reduce this strain.
Elevate Your Legs: When you have a moment, prop your legs up above the level of your heart for 15-20 minutes. This simple action uses gravity to your advantage, helping drain pooled blood and relieve pressure.
Wear Compression Stockings: Especially if your job involves prolonged sitting or standing, these garments provide gentle pressure to help your veins and calf muscles move blood more efficiently.
Protect Your Skin from the Sun: UV damage breaks down collagen, the protein that gives structure to your skin and blood vessel walls. Weakened vessel walls are more susceptible to becoming spider veins. For more, check our guide on sunscreen myths and evidence-based facts every St. Louis resident should know.
At our St. Louis dermatology practice, Dr. Gibstine often tells patients, "Prevention is about consistency. Wearing compression stockings on a long workday or remembering to take a walk during your lunch break does more for your veins than any single, isolated action."
When to See a St. Louis Dermatologist About Your Spider Veins
For most people, spider veins are a cosmetic concern. However, it's crucial to pay attention to how your legs feel, not just how they look. Sometimes, those visible veins hint at a more significant venous problem lurking beneath the surface.
If you’re dealing with a persistent ache, throbbing, or a constant feeling of heaviness in your legs, it’s a good idea to get a professional opinion.
Symptoms That Shouldn't Be Ignored
Here at Mid-County Dermatology, serving communities from Clayton to Ladue, we always tell our patients to book a visit if their spider veins are accompanied by any of the following signs:
Swelling: Noticeable puffiness in your legs or ankles, particularly at the end of the day.
Aching or Pain: A constant, nagging ache, throbbing, or burning feeling directly over the veins.
Skin Changes: Skin near the veins that looks darker, feels leathery, or becomes dry and itchy.
Spontaneous Bleeding: Veins that bleed from a minor bump or for no apparent reason require immediate attention.
These symptoms suggest the pressure inside your veins is affecting the surrounding tissue. That’s when an evaluation by a St. Louis skin specialist becomes essential.
Of course, getting the right diagnosis starts with finding a reputable dermatologist you trust. Our guide on how to find a St. Louis dermatologist has some great tips. If any of this sounds familiar, don't wait and worry. Dr. Feigenbaum and Dr. Gibstine are here to provide a clear diagnosis and a personalized care plan.
Key Takeaways
The primary cause of spider veins is venous insufficiency, where tiny valves in the veins fail.
Major risk factors include genetics, hormonal shifts, aging, and lifestyle habits like prolonged standing.
Most spider veins are a cosmetic issue, but symptoms like pain, swelling, or skin changes warrant a visit to a dermatologist.
Lifestyle changes like exercise, weight management, and elevating your legs can help prevent new spider veins.
Professional treatments like sclerotherapy are safe, effective, and minimally invasive for removing existing spider veins.
Frequently Asked Questions About Spider Veins
Here are answers to some of the most common questions our team at Mid-County Dermatology hears from patients across the St. Louis area, from Ladue to Chesterfield.
What Is the Difference Between Spider Veins and Varicose Veins?
The biggest difference is their size and depth. Spider veins are tiny, fine lines right at the skin's surface, usually red, blue, or purple. They are typically a cosmetic concern and don't cause pain. Varicose veins are much larger, deeper, bulging, rope-like cords that are more likely to cause symptoms like aching, throbbing, or heaviness and can signal a more significant underlying vein issue.
Are Treatments for Spider Veins Painful?
Modern spider vein treatments are minimally invasive with very little discomfort. Most patients describe sclerotherapy—the most common treatment—as feeling like a series of tiny pinpricks. Laser therapy might feel like a small rubber band snapping against your skin. Our St. Louis skin specialists prioritize your comfort throughout the entire process.
Does Insurance Cover Spider Vein Treatment?
Insurance coverage depends on whether the treatment is cosmetic or medically necessary. If your spider veins are purely a cosmetic issue, insurance typically won't cover removal. However, if they are linked to symptoms of venous disease—like pain, significant swelling, or skin ulcers—the treatment may be considered medically necessary and could be covered. We suggest checking with your provider; our office can help you navigate your benefits.
Can Spider Veins Come Back After Treatment?
While treatments effectively eliminate the targeted veins, they cannot prevent new ones from forming. If you have a strong genetic predisposition, new spider veins may appear over time. This is why maintaining a healthy lifestyle, including regular exercise and managing your weight, is so crucial for long-term vein health. You may need follow-up treatments over the years.
To learn more about the full range of conditions we manage, check out our complete guide on what a dermatologist treats.
Ready to address your spider veins with expert care? The board-certified team at Mid-County Dermatology is here to create a personalized treatment plan for you. Schedule your consultation today by visiting https://www.midcountyderm.com.
This information is for educational purposes only and does not constitute medical advice. Please consult with Dr. Feigenbaum, Dr. Gibstine, or another qualified healthcare provider at Mid-County Dermatology for personalized treatment recommendations. Individual results may vary.
